By Govind Pawar, Senior Clinical Operations Leader, Oxygen Clinical Research and Services
Clinicaltrial Myths India Patients. As India’s pharmaceutical and biotechnology sectors race toward cutting-edge therapies—ranging from novel cancer drugs to gene therapies and vaccines—clinical trials remain the gold standard for evaluating safety and efficacy. Despite regulatory reforms, improved ethical oversight, and high-profile successes such as indigenous COVID-19 vaccine candidates, patient trust in clinical research continues to lag. However, this gap highlights a deeper issue of perception and awareness. Moreover, when these myths are left unchecked, they do more than just slow recruitment. In fact, they actively hinder India’s progress as a global destination for responsible and world-class medical research. Therefore, addressing these misconceptions is not just important but essential for the future of clinical trials in India.
In this opinionated report, we explore the most persistent patient myths, examine their roots and suggest practical steps to bridge the information gap—because understanding is the first step toward empowerment.
Myth #1: “In Clinical Trials, You’re Just a Guinea Pig”
The image of desperate volunteers strapped to an operating table, their bodies dissected for corporate profit, is a trope as old as research itself. Among many Indian patients, the fear persists that participation in a trial equates to involuntary experimentation, with little regard for their well-being. Newspapers occasionally highlight tragic accidents or allegations of consent violations.
As a result, these reports reinforce the perception that clinical trials are inherently dangerous. Moreover, such coverage contributes to the spread of misinformation and strengthens existing fears among potential participants.
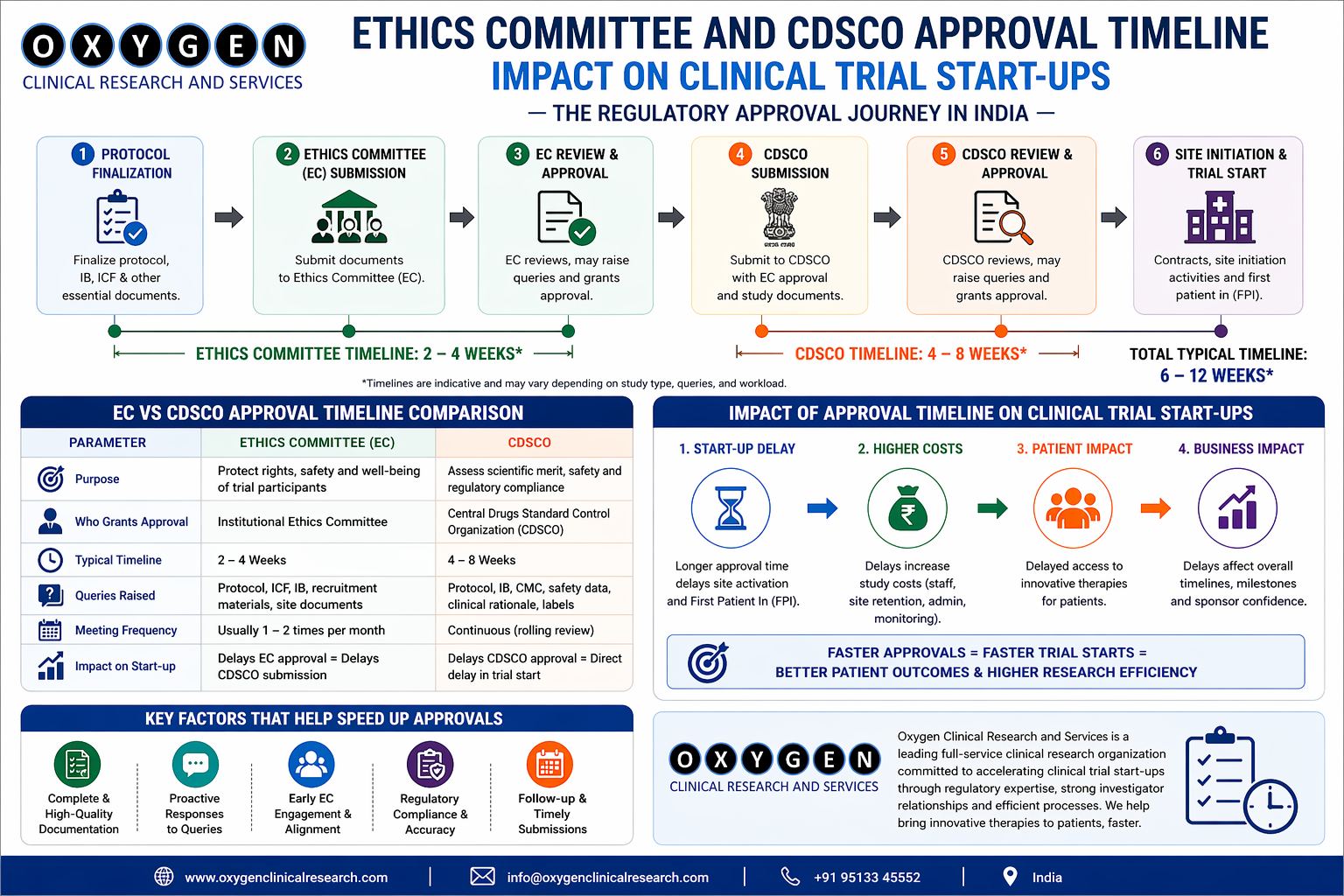
Reality Check: India’s regulatory framework for clinical trials has been overhauled in recent years. The New Drugs and Clinical Trials Rules, 2019, introduced stringent timelines for regulatory decisions and mandated robust informed-consent procedures. Every trial proposal must pass scrutiny by an ethics committee registered with the Central Drugs Standard Control Organisation (CDSCO). These committees include medical experts, legal advisers and independent members to protect participants’ rights and safety.
Myth #2: “Only the Poor and Illiterate Volunteer for Research”
A second misconception paints trial volunteers as socioeconomically vulnerable: uneducated villagers who are lured by small incentives, unaware of potential risks. This stereotype not only stigmatizes participants from all walks of life but also overshadows the fact that many middle-class urbanites, chronically ill patients and patient-advocacy groups actively engage in research.
Reality Check: Clinical-trial participation in India spans a broad demographic spectrum. In metropolitan cities, tech-savvy patients with online access to clinical-trial registries voluntarily enroll in phase II and III trials of oncology, neurology and rare diseases. Many rare-disease support groups not only educate members about ongoing research but also collaborate directly with investigators. The government’s Clinical Trials Registry–India (CTRI) database is freely accessible online, enabling patients to search by disease category, trial phase and location. Increasingly, private hospitals in Tier II and III cities host well-monitored trials, with institutional ethics committees and standalone data-monitoring boards.
Myth #3: “Pharma Companies Only Care About Profit, Not Patients”
Many people believe that pharmaceutical companies focus only on profit.
They think these companies promote unsafe or incomplete drugs in India.
This belief comes from the idea that regulations are weak.
It also assumes that trial participants are easy targets.
Some even feel that foreign sponsors exploit these gaps.
They believe India is used as a testing ground for drugs.
These include antibiotics, antiretrovirals, and vaccines.
They assume such drugs would not pass safety checks in Western countries.
Reality Check:
Some isolated incidents have occurred in the past.
However, making broad generalizations is not helpful. Multinational companies follow international guidelines—including Good Clinical Practice (GCP) standards—and often submit the same protocols for global approval. In fact, data from Indian trial sites have contributed to global approvals of blockbuster drugs and transformed standards of care. The narrative that “all trials here are second-rate” ignores the growing cadre of world-class researchers based in India.
Myth #4: “You’ll Never Get Follow-Up Care or Compensation”
Another pervasive fear is that once the trial is over, participants are often cast aside and left without adequate medical support or long-term monitoring. Moreover, concerns about the lack of recourse for potential side effects further intensify this perception. As a result, such beliefs continue to reinforce common clinical trial myths in India and discourage patient participation.
Skeptics point to confusion over compensation rules, believing that if they suffer harm, there is no mechanism for redress.
Reality Check: Compensation provisions are built into Indian regulations. The New Drugs and Clinical Trials Rules stipulate a compensation formula for trial-related injury or death, calculated on the basis of age, risk and medical costs. Sponsors must create a compensation fund and deposit the required amount before enrolment begins. Additionally, ethics committees oversee insurance coverage and follow-up requirements, ensuring that participants receive medical care until their condition stabilizes.
Myth #5: “Clinical Trials Are Always Conducted in Big Cities, Excluding Rural India”
Many patients in small towns and villages believe that trials are the preserve of large urban hospitals, with rural and tribal populations cut off from potential benefits.
This disconnect feeds mistrust: if communities never see research happening locally, they assume it’s “not for us.”
Reality Check: India’s clinical-trial footprint has expanded well beyond big metros. With the government’s push to decentralize research, accredited clinics now exist in district hospitals, community health centres and private nursing homes across multiple states. Mobile clinical-trial units bring diagnostic facilities and trained personnel to remote areas, reducing travel burdens Clinicaltrial Myths India Patients.
Why These Myths Persist
- Low Awareness Levels: Despite the availability of online registries and patient-education resources, penetration is limited. In rural areas, literacy rates and lack of internet access hinder outreach efforts.
- Media Sensationalism: High-profile stories of adverse events or legal battles often overshadow routine trial successes, creating a skewed narrative.
- Language and Cultural Barriers: Informed consent forms are typically drafted in English or in formal Hindi, alienating speakers of regional languages and dialects.
- India’s colonial past has significantly shaped public perception of healthcare initiatives. Moreover, experiences with unregulated medical campaigns, such as unauthorized drug distribution, have deepened mistrust among communities. As a result, there remains a lingering skepticism toward externally sponsored health programs. Therefore, addressing these historical concerns is essential to building trust in modern clinical research.
- Inconsistent Communication: Investigators and sponsors sometimes prioritize recruitment over continuous engagement, failing to update participants on trial progress or outcomes.
The Stakes Are High
Without public trust, India risks:
- Slower Patient Recruitment.
- Delays in Novel Therapy Approvals.
- Reduced Foreign Investment in Clinical Research.
- Limited Access to Cutting-Edge Treatments for Indian Patients.
If India aspires to compete globally in medical innovation, dispelling these myths cannot remain an afterthought. A robust R&D ecosystem demands an informed, willing participant base.
Bridging the Information Gap: A Roadmap
- Simplify Informed Consent
- Translate consent forms into local languages.
- Use visual aids—infographics, short videos—that explain trial phases, potential benefits and risks.
- Conduct consent discussions in a private, culturally sensitive environment.
- Strengthen Community Engagement
- Partner with local NGOs, patient-advocacy groups and primary-care doctors to disseminate accurate information.
- Organize “trial-awareness” camps in rural districts, with case studies of successful patient outcomes.
- Leverage Digital Platforms
- Develop mobile apps that list ongoing trials, eligibility criteria and contact details in multiple languages.
- Use SMS alerts to keep enrolled participants informed about appointments, lab results and study updates.
- Reform Media Narratives
- Encourage responsible reporting by providing journalists with contextual data and expert contacts.
- Highlight positive success stories—such as rare-disease patients who benefitted from trial drugs now available in the market.
- Empower Ethics Committees
- Allocate resources for periodic site audits, especially at remote clinics.
- Facilitate training workshops on cultural sensitivity and communication skills.
- Introduce Patient Advocates
- Mandate the presence of an independent patient advocate or liaison in every trial site to address participants’ concerns in real time.
Voices from the Field
Dr. Nandini *** ****, Chairperson of the State Ethics Review Board in Karnataka, shares her perspective.
“Our biggest challenge isn’t scientific. It’s social.” We have the infrastructure and the expertise.
Ramesh *** *****, a 58-year-old patient with chronic kidney disease from Meerut, shares his experience.
“When my doctor first suggested a trial for a new dialysis adjunct, I was terrified.”
. I had read stories online about trials gone wrong. Only after meeting the research team did I feel more confident.
I also spoke with other participants, and as a result, I gradually gained confidence in the entire process. Subsequently, I realized that the trial was not only safe but also professionally managed. Consequently, my initial fears began to fade. Now, I feel better than I have in years. Overall, this experience has helped me overcome common clinical trial myths in India while also building lasting trust in the system.
Conclusion: Building Trust as a Collective Responsibility
Clinical trials are neither charity nor covert exploitation; they are the engine of medical progress. India’s regulators, researchers and sponsors have made substantial strides in ensuring ethical conduct and patient protection. What remains incomplete is the connection between the trial site and the community.
In other words, this gap needs a strong bridge.
This bridge should be built on transparent communication and genuine engagement.
Most importantly, it must respect participants as partners, not just subjects.
Only by confronting these misconceptions can India build a stronger research ecosystem.
This ecosystem can drive global innovation.
It can also protect the dignity and safety of every volunteer. Moreover, addressing these concerns helps dispel common clinical trial myths in India. As a result, patients feel more confident and informed when participating in clinical research.