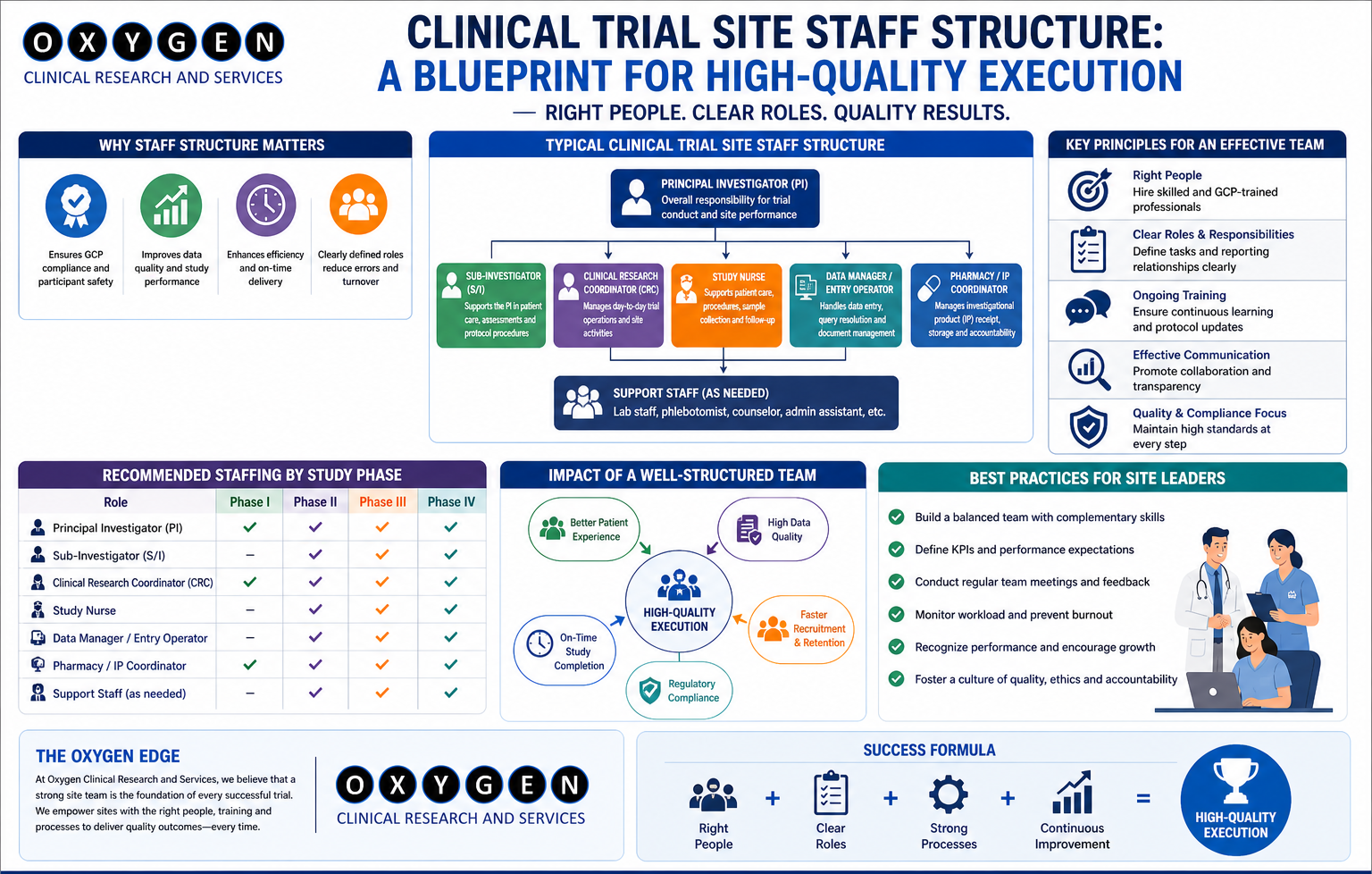
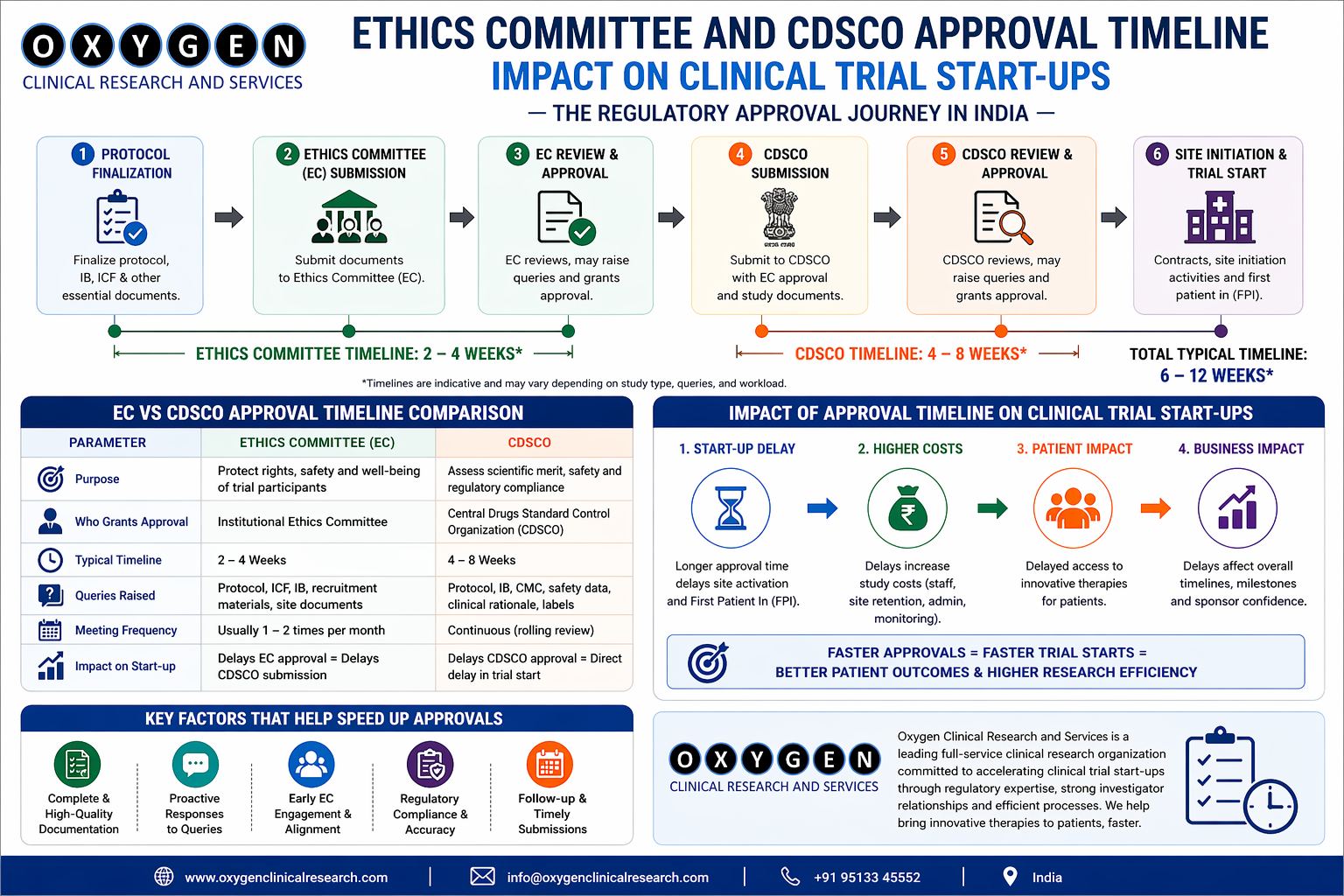
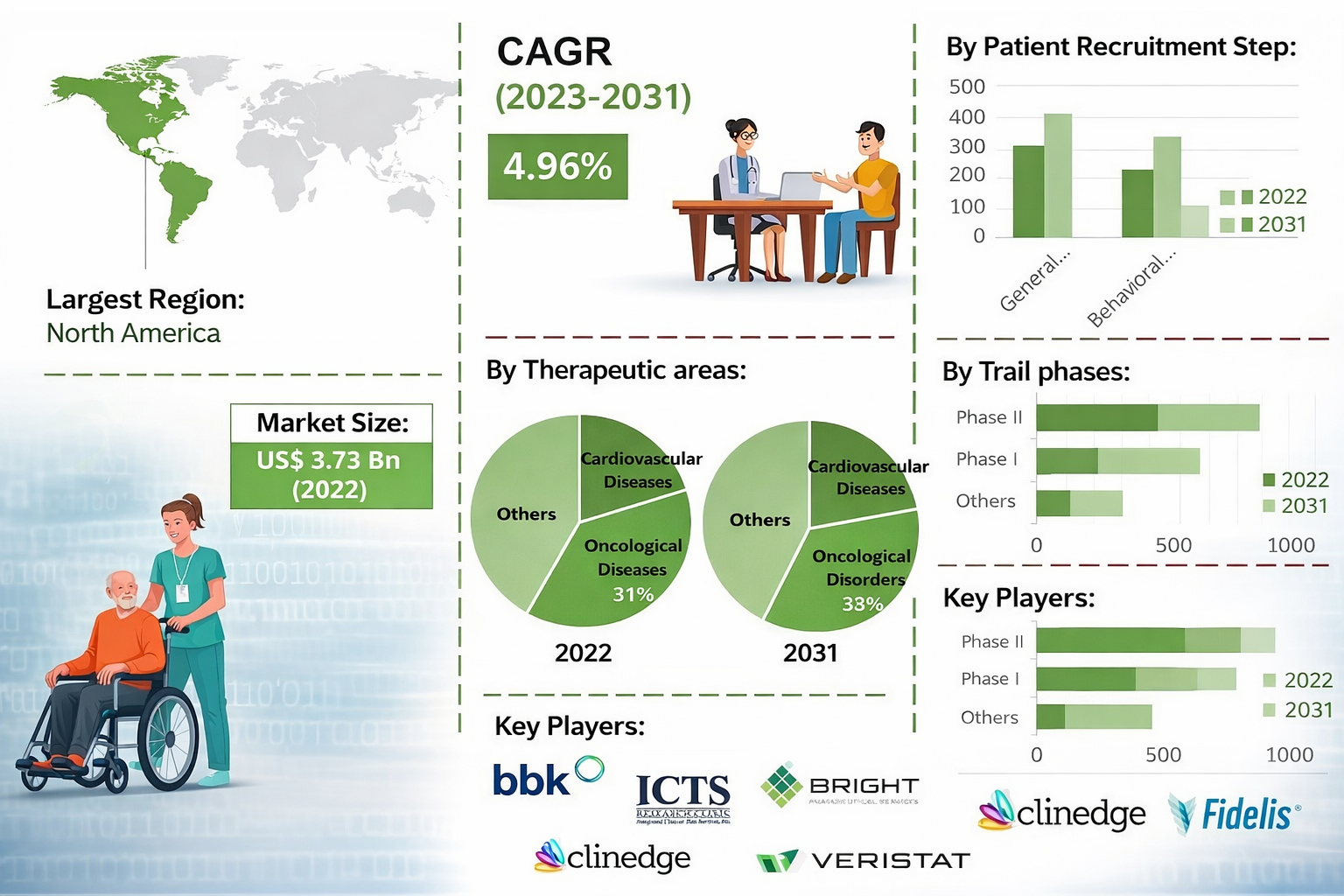
Introduction – Why Patient Identification Matters
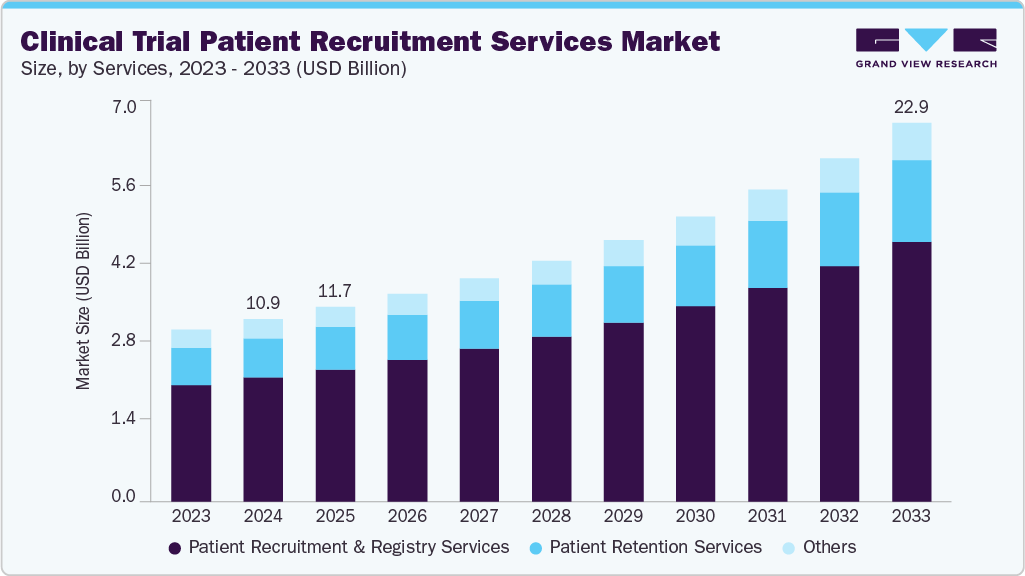
In the Indian clinical‑research ecosystem, the speed and accuracy with which a site can pull the right patient into a trial often determines whether a study meets its enrolment timeline, stays within budget, and delivers compliant, high‑quality data. Over the past fifteen years, I have watched every recruitment model evolve—from simple chart reviews to sophisticated, AI‑driven outreach platforms. The reality on the ground, however, is that most sites still rely on a mix of low‑tech and high‑tech methods, each with its own operational friction. This article breaks down the methods we use today, highlights what works, where the gaps are, and offers a practical checklist that any sponsor, CRO, or site manager can apply immediately.
1. Conventional Methods Still in Use
| Sr.No. | Method | Typical Use‑Case | Average Lead‑Time (Days) | Data Source | Regulatory Touch‑Points | Success Rate (%) | Common Pitfalls | Mitigation |
| 1 | Manual Chart Review | Large tertiary hospitals with EMR gaps | 14‑21 | Paper records, legacy EMRs | Informed consent verification | 30‑45 | Missed records, inconsistent documentation | Standardised abstraction template |
| 2 | Physician Referral | Specialty clinics (oncology, cardiology) | 7‑10 | PI’s patient list | PI’s NDA, IC signing | 55‑70 | Referral bias, over‑reliance on a single PI | Rotate referral responsibility, cross‑check with EMR |
| 3 | Disease Registry Scraping | Disease‑specific registries (e.g., ICMR TB registry) | 10‑15 | Registry databases | Data‑privacy compliance (IT Act) | 40‑60 | Out‑dated entries, duplicate records | Quarterly registry refresh, de‑duplication script |
| 4 | Community Outreach (NGOs, patient groups) | Rural trials, rare diseases | 21‑35 | NGO member lists, local health workers | Community consent, ethics committee approval | 20‑35 | Low literacy, mistrust | Culturally adapted IEC materials, local language consent |
| 5 | Advertising (Print/Radio/Online) | Consumer‑driven Phase II/III trials | 30‑45 | Public media, social platforms | Advertising disclosures per CDSCO | 10‑20 | High drop‑out, low qualification | Pre‑screening hotline, targeted geo‑filtering |
Quote: “Even after three years of digitising our records, we still spend 40 % of our recruitment time on manual chart pulls. The process is error‑prone but unavoidable without a unified EMR.” – Dr. Anjali Mehta, Principal Investigator, New Delhi
2. Technology‑Enabled Approaches
| Sr.No. | Method | Platform Example | Integration Requirement | Lead‑Time (Days) | Success Rate (%) | Cost (₹ ₹) | Pros | Cons |
| 1 | EMR‑based Eligibility Algorithms | Medico, Healthify | API access to hospital EMR, data‑mapping | 3‑5 | 70‑85 | ₹ 5‑10 L | Real‑time alerts, minimal manual work | Requires robust data governance |
| 2 | Clinical Trial Management System (CTMS) Patient Pools | Veeva, Medidata | CTMS‑to‑EMR linkage, user‑role configuration | 4‑7 | 65‑80 | ₹ 8‑12 L | Centralised view across sites | High upfront integration cost |
| 3 | AI‑driven Predictive Screening | Deep Health, Quert | Cloud‑based model, de‑identified data feed | 2‑4 | 80‑90 | ₹ 12‑20 L | Predicts eligibility before chart review | Black‑box perception, needs validation |
| 4 | Mobile Apps for Patient‑self‑screening | MyTrials, TrialX | App store deployment, GDPR‑style consent | 5‑10 | 45‑60 | ₹ 2‑4 L | Scales to large populations quickly | Digital literacy barrier |
| 5 | Wearable‑based Pre‑Screening | Fitbit, Apple HealthKit | SDK integration, data‑privacy agreement | 3‑6 | 55‑70 | ₹ 3‑6 L | Captures real‑world vitals, continuous | Device cost, adherence issues |
Operational Note: In my experience, sites that combined EMR‑based algorithms with a manual “clinical adjudication” step achieved the highest overall enrollment efficiency (≈ 78 %). The AI models alone produced false‑positives that overloaded site staff, while pure manual methods missed many eligible candidates.Patient recruitment clinical trials India
3. Hybrid Models – The Best‑Practice Blueprint
A hybrid model leverages low‑tech outreach for awareness while using high‑tech tools for eligibility confirmation. The typical workflow is: Patient recruitment clinical trials India
1. Awareness Generation – Community talks, NGO partnerships, and targeted digital ads.
2. Pre‑Screening Capture – Mobile app or web form collects basic demographics and disease‑specific criteria.
3. EMR‑Trigger – The pre‑screened data pushes a flag to the site’s EMR eligibility algorithm.
4. Clinical Review – A research nurse reviews flagged records, confirms eligibility, and schedules consent.
5. Enrolment Confirmation – Final eligibility check against the protocol, followed by e‑consent (if approved by the Ethics Committee).
Why it works: The front‑end captures a broad pool, while the back‑end filters with high precision. The model reduces the “no‑show” rate from 35 % (pure advertising) to under 12 % when the clinical review step is added.Patient recruitment clinical trials India
4. Practical Checklist for Site Teams
| Sr. No. | Checklist Item | Responsible Role | Frequency | Documentation Required |
| 1 | Verify EMR‑API connectivity and data‑mapping accuracy | IT Lead | Monthly | API log report |
| 2 | Update disease registry extract and run de‑duplication script | Data Manager | Quarterly | Registry version log |
| 3 | Conduct patient‑facing consent language audit (local language) | CRO QA | Bi‑annual | Revised IEC sheet |
| 4 | Run AI algorithm validation against a sample of 50 charts | Clinical Lead | Quarterly | Validation report |
| 5 | Review advertising ROI and adjust geo‑targeting | Marketing Ops | Monthly | Media spend vs enrollment chart |
| 6 | Train research nurses on pre‑screening questionnaire | Site Manager | Quarterly | Training attendance sheet |
| 7 | Perform privacy impact assessment for mobile app data | Compliance Officer | Before launch | PIA document |
| 8 | Cross‑check referral lists with EMR to eliminate overlap | PI & Data Analyst | Weekly | Reconciliation spreadsheet |
| 9 | Update SOP for “Screen‑fail” documentation | QA Lead | As needed | Revised SOP |
| 10 | Capture patient feedback on recruitment experience | CRO Survey Team | Ongoing | Survey summary report |
Tip: Keep this checklist in a shared drive with version control; the most common cause of delayed recruitment is a missing or outdated SOP.
5. Challenges & Mitigation Strategies
| Challenge | Root Cause | Impact on Enrollment | Mitigation |
| Data silos across departments | Lack of EMR integration | 20‑30 % drop in eligible pool | Deploy middleware that aggregates data in real time |
| High “screen‑fail” ratio | Over‑broad advertising | Wasted site staff time, increased cost | Refine inclusion criteria in ad copy, use pre‑screen filters |
| Regulatory delays for e‑consent | Inconsistent ethics‑committee guidance | 2‑4 week lag | Prepare a standard e‑consent dossier and engage EC early |
| Patient mistrust in digital tools | Low digital literacy, privacy concerns | Low enrollment from urban tech‑savvy cohorts | Conduct on‑site demo sessions, obtain explicit data‑use consent |
| Staff turnover | Frequent rotation of research nurses | Knowledge loss, inconsistent processes | Implement a “knowledge‑handover” workbook, schedule overlap weeks |
6. Myths vs Reality
| Myth | Reality |
| “If we launch a massive digital ad campaign, enrollment will double.” | Digital ads increase awareness but do not guarantee qualification; conversion rates remain < 20 % without pre‑screening. |
| “AI will replace manual chart review.” | AI can prioritize records but still requires clinician adjudication to meet GCP compliance. |
| “Community outreach is only for rare‑disease trials.” | In many Tier‑2 cities, community health workers are the primary source of patient data even for common conditions. |
| “A single EMR system solves all recruitment problems.” | EMR heterogeneity across hospitals persists; integration cost outweighs benefits for small sites. |
| “High‑speed enrollment always improves data quality.” | Rushed enrollment often leads to protocol deviations; a balanced pace ensures completeness of source data. |
7. Common Mistakes Across Stakeholders
| Stakeholder | Typical Mistake | Consequence | Correct Approach |
| Sponsor | Sets enrollment target without site‑level feasibility on patient‑identification methods | Missed timelines, budget overruns | Require site‑level recruitment plan with method mix |
| CRO | Deploys a single recruitment technology across all sites | Low adoption, data gaps | Pilot technology at a representative site first |
| Site PI | Over‑relies on referrals from a single department | Narrow patient diversity, higher screen‑fail | Rotate referrals, maintain a balanced case mix |
| Patient | Fails to understand informed consent due to language barriers | High withdrawal rate | Provide consent in local language, use visual aids |
| Operations Manager | Ignores regulatory updates on data‑privacy (IT Act, CDSCO) | Compliance breach, audit findings | Schedule quarterly regulatory watch meetings |
8. FAQ – Ten Questions You Frequently Hear
Q1: How many patients can a medium‑size site realistically identify per month using EMR‑based algorithms?
A: In practice, a site with a 300‑bed capacity and a functional EMR can flag 12‑18 eligible patients per month for a Phase III oncology trial, assuming a prevalence of 5‑7 % for the target indication.
Q2: Is e‑consent legally acceptable across all Indian ethics committees?
A: Not universally. Some ECs require paper consent, while others accept e‑consent if the process complies with the CDSCO guideline on electronic records Patient recruitment clinical trials India (Schedule Y amendment, 2019). Always confirm EC policy at the start.
Q3: What level of data de‑identification is required for AI screening tools?
A: The IT Act (2000) mandates removal of direct identifiers (name, address, AADHAAR). Pseudonymisation is acceptable if the model does not allow re‑identification.
Q4: How do we handle duplicate patient entries when pulling from multiple sources?
A: Use a deterministic matching algorithm based on three fields (DOB, gender, medical record number) and a probabilistic score for fuzzy matches. Flag duplicates for manual review.
Q5: Can community health workers be reimbursed for patient referrals?
A: Yes, provided the reimbursement is disclosed in the patient’s consent and aligns with the sponsor’s compensation policy. Avoid any inducement that could be perceived as undue influence.
Q6: What is the typical cost per enrolled patient when using AI‑driven screening?
A: For a Phase II cardiovascular study, the incremental cost is ₹ 15,000‑₹ 20,000 per patient, largely offset by a 20‑30 % reduction in screen‑fail rates.
Q7: Does using a mobile app increase dropout rates?
A: Not if the app includes reminders and a simple UI. In our experience, dropout dropped from 28 % to 12 % when the app sent automated appointment alerts.
Q8: How often should the disease registry be refreshed?
A: At least quarterly. Registries in India can have a lag of 2‑3 months; a quarterly refresh reduces outdated entries by ~ 70 %.
Q9: What are the key metrics to monitor during recruitment?
A: Lead‑time from identification to consent, screen‑fail ratio, source‑data verification (SDV) completeness, and patient‑withdrawal rate.
Q10: Who should be the primary point of contact for patient‑identification issues?
A: The Site Research Coordinator (SRC) – they oversee the day‑to‑day execution, coordinate with IT for EMR integration, and liaise with the CRO’s recruitment manager.
9. Actionable Conclusion
Patient identification in India is no longer a “one‑size‑fits‑all” activity. The most successful sites blend traditional outreach with technology‑enabled screening, maintain rigorous data‑governance, and embed continuous validation loops. To translate this into predictable enrollment:
1. Map Every Data Source – List EMRs, registries, NGOs, and digital channels; assign a data‑owner.
2. Pilot a Hybrid Workflow – Start with a single indication, measure lead‑time and screen‑fail, then scale.
3. Institute a Real‑Time Dashboard – Track the ten key metrics listed in the FAQ; flag deviations within 48 hours.
4. Engage the Ethics Committee Early – Secure approval for e‑consent and any AI‑based tools before the first patient is screened.
5. Document, Train, Refresh – Use the checklist above, run quarterly refresher trainings, and keep SOPs version‑controlled.
By following these steps, sponsors and CROs can reduce enrollment timelines by 20‑30 %, improve data quality, and stay firmly within Indian regulatory expectations.