Clinical Trial Staff Structure. Most clinical trial delays in India do not stem from a lack of patients; they stem from a lack of bandwidth at the site level. When I review failed timelines, the common denominator is almost always an under-resourced site team, where the Principal Investigator (PI) is distracted by clinical practice and the study coordinator is overwhelmed by administrative burden. If you are a sponsor or a CRO leader, you know the cost of a site falling behind. It is not just the burn rate of the site; it is the delay in your global submission, the integrity of your data, and the potential for a disastrous audit. After 15 years in the field, I have realized that the site staff structure is the most critical variable in the trial success equation.
The following comparison highlights the impact of site staffing models on key trial metrics.
| Sr No | Role Structure | Budget Impact | Start-up Speed | Data Quality | Audit Risk | Protocol Adherence | Staff Turnover | Patient Retention | Monitoring Load |
| 1 | Full-time Dedicated | High | Fast | High | Low | Excellent | Low | High | Medium |
| 2 | Part-time Shared | Medium | Moderate | Medium | Medium | Good | Moderate | Medium | High |
| 3 | Minimalist/PI-led | Low | Slow | Low | High | Poor | High | Low | Very High |
| 4 | Hybrid (CRO-funded) | High | Fast | High | Low | Excellent | Low | High | Medium |
| 5 | Outsourced Support | Medium | Moderate | Medium | Medium | Moderate | High | Moderate | High |
The Reality of Site Staffing in India
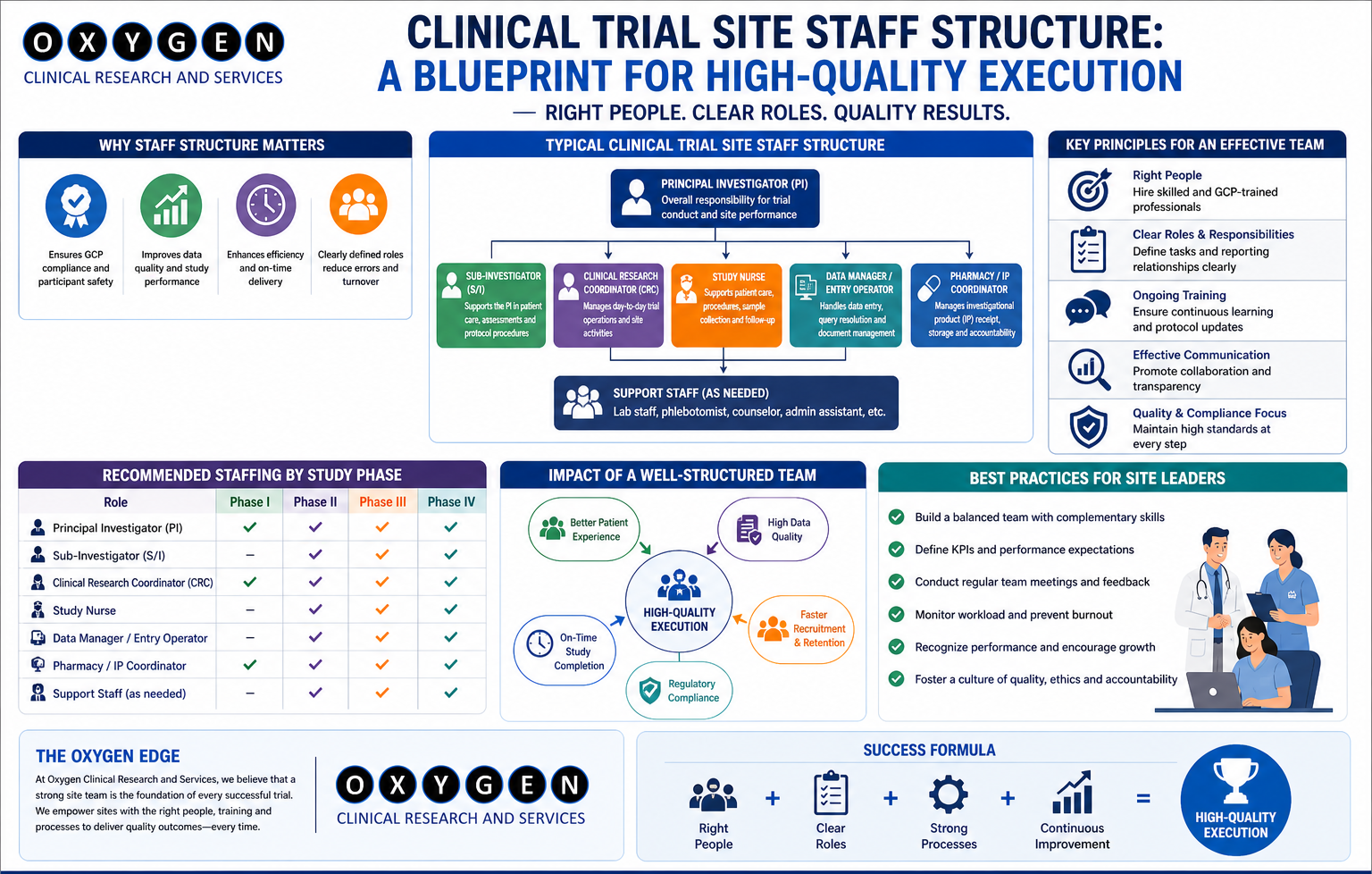
Under the New Drugs and Clinical Trials Rules (2019), the responsibility of the PI is absolute. However, the operational execution is delegated. A standard, high-performing site team in India requires more than just a PI and a coordinator.
Essential Roles for Execution
- Principal Investigator (PI): Overall accountability and medical oversight.
- Clinical Research Coordinator (CRC): Data entry, patient scheduling, and regulatory document maintenance.
- Pharmacist: Strict drug accountability, temperature log maintenance, and IP management.
- Laboratory Technician: Sample processing, storage, and shipment management (often the bottleneck in PK studies).
- Regulatory/QA Associate: Ethics Committee (EC) submissions and site-level compliance.
When these roles are collapsed—for example, when a single person handles both IP management and patient recruitment—data quality suffers. We see this often in clinical trial site management in India.
Operational Bottlenecks: Where Projects Fail
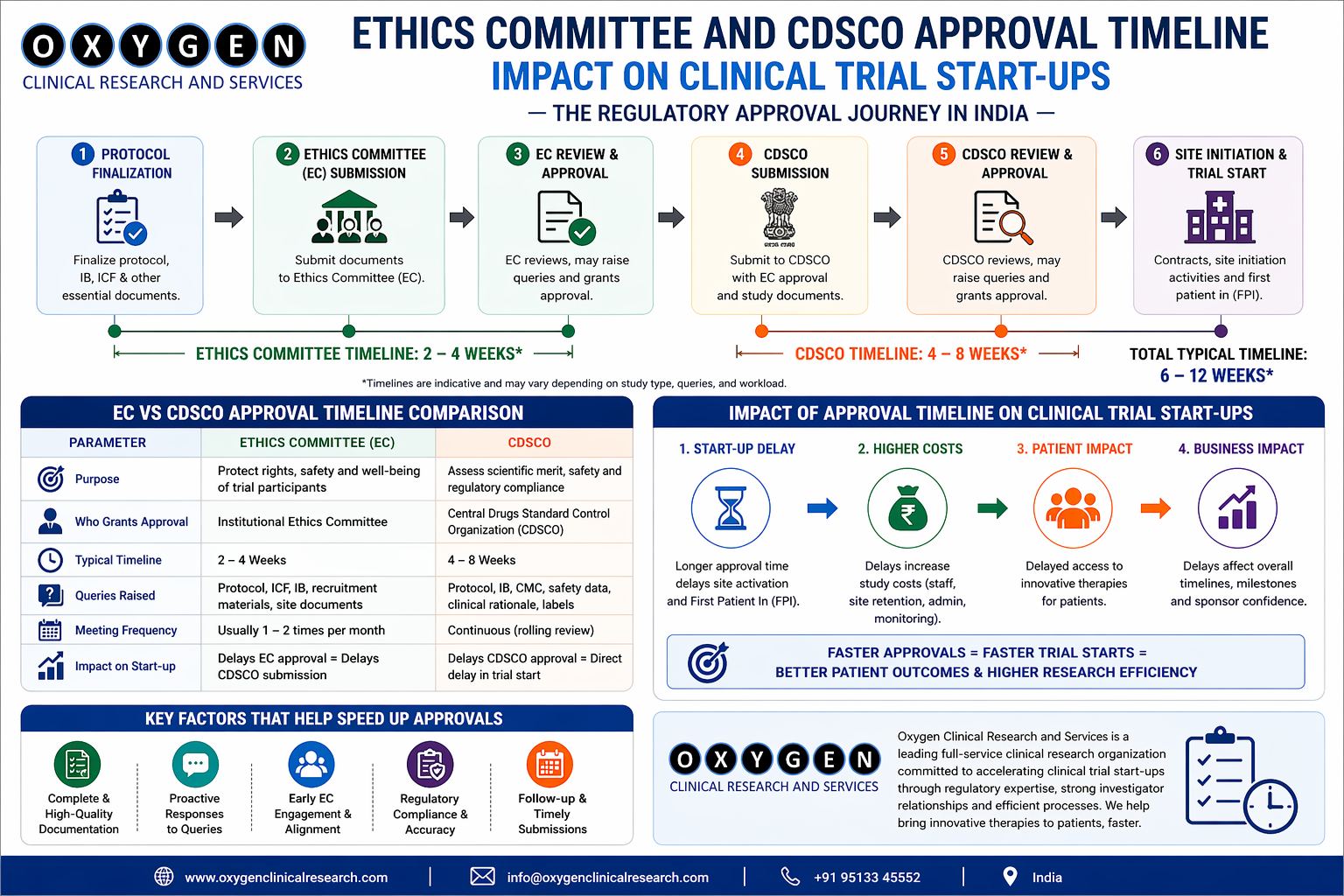
Delays occur at the intersection of regulatory compliance and site workload. CDSCO and EC submissions are rigorous. If your site team is focused only on patient visits, the regulatory paperwork—the foundation of your trial—will lag.
Table 2: Common Operational Failures at Site Level
| Sr No | Process Area | Typical Delay | Impact on Trial | Root Cause | Risk Level | Mitigation Strategy | Cost Overrun |
| 1 | EC Approval | 4–6 weeks | Start-up | Incomplete docs | High | Proactive review | Low |
| 2 | IP Management | Ongoing | Compliance | Poor documentation | Critical | Dedicated staff | Moderate |
| 3 | Data Entry | 2+ weeks | Query load | Staff bandwidth | Medium | Real-time monitoring | High |
| 4 | Patient Consent | Daily | Ethics | Hurried process | Critical | Training/Audit | High |
| 5 | Lab/Sample | Ongoing | Data loss | Improper logs | Critical | Standardized SOPs | High |
Case Studies: Real-World Execution Insights
Case 1: The Overloaded Coordinator
- Study: Phase III Oncology.
- Problem: 22% data query rate; 3-month recruitment delay.
- Root Cause: One coordinator managing two high-volume studies.
- Action: Recruited a dedicated assistant coordinator for data entry.
- Outcome: Query rate dropped to 4% within 60 days.
- Lesson: Never assume a coordinator can scale linearly with patient volume.
Case 2: The Regulatory Bottleneck
- Study: Phase II Cardiology.
- Problem: Site could not start for 5 months post-site selection.
- Root Cause: PI was handling EC submissions; hospital admin was unresponsive.
- Action: Hired an external regulatory liaison to manage hospital/EC tracking.
- Outcome: Approval received in 45 days.
- Lesson: Administrative hurdles are often external to the research team.
Case 3: The IP Compliance Breach
- Study: Rare Disease.
- Problem: Temperature excursions ignored.
- Root Cause: No dedicated pharmacist; nurse was “managing” IP.
- Action: Implemented a mandatory site-level pharmacy role.
- Outcome: 100% compliance in last two audits.
- Lesson: IP management should never be a secondary responsibility.
Challenges and Mitigation: The Hard Truth
Most sponsors try to save costs by minimizing site staff. This is a false economy. A site with a lean, overworked team will require more monitoring visits (CRAs), more data cleaning, and potentially more site management travel. My experience at Oxygen Clinical Trial shows that investing in the right headcount at the start prevents expensive “firefighting” later.
Myths vs. Reality
- Myth: An experienced PI can run a site without dedicated staff.
- Reality: Even the best PI needs a strong operational backbone to handle GCP-compliant documentation.
- Myth: CROs always provide the best site staff.
- Reality: High-turnover environments in large CROs often leave sites with inexperienced personnel.
Practical Sponsor Checklist
Feasibility Stage
- Verify the PI’s current clinical load.
- Audit the proposed site staff-to-patient ratio.
- Ensure the site has a dedicated space for monitoring and record-keeping.
Startup Stage
- Review the Delegation of Authority log for clarity.
- Ensure the pharmacist is trained on the specific IP requirements.
- Check that regulatory staff have a timeline for EC/DCGI renewals.
Execution Stage
- Conduct “spot checks” on data entry timelines.
- Review staff turnover rates at the site.
- Assess if the clinical research services in India provided meet the study’s complexity.
Regulatory Context: CDSCO and Global Standards
Compliance with the New Drugs and Clinical Trials Rules (2019) is non-negotiable. Your site staff must be trained on ICH-GCP E6(R3) and understand the implications of non-compliance for both the sponsor and the investigator. Periodic review of CTRI registration and adherence to EC conditions is where many projects fail during inspections.
FAQ: Clinical Operations Insights
- What is the ideal patient-to-coordinator ratio? In complex oncology or rare disease trials, the ratio should not exceed 1:10. For simpler, chronic condition trials, 1:20 is manageable. Anything higher risks data quality.
- Should the sponsor fund site staff directly? Yes. In the Indian context, “site-funded” staff are often shared with the hospital’s clinical practice, meaning the trial takes a backseat when the hospital is busy. Dedicated, sponsor-funded staff protect your timeline.
- How do you handle high staff turnover at sites? Build a buffer in your budget for training. Create a standard “Site Operations Manual” that makes onboarding new staff faster and keeps the process standardized Clinical Trial Staff Structure.
- What is the biggest mistake in site selection? Ignoring the “hidden” hospital administration constraints. A site may have a great PI, but if the hospital contract process takes six months, your trial is dead on arrival.
Why does site monitoring often fail at the start? Lack of alignment on expectations. The CRA expects the site to be ready, but the site lacks the administrative support to prioritize the CRA’s requests Clinical Trial Staff Structure.
Conclusion
Effective site staff structure is the difference between a high-quality data set and a regulatory warning letter. If you are struggling with site performance or want to ensure your next study in India is executed with precision, let’s discuss your operational strategy.
For site management support, you can reach out directly at govindpawar@oxygenclinicaltrials.com or connect with me on LinkedIn. You can also learn more about our approach at Oxygen Clinical Trial. For specific inquiries, use our contact page.